By Beatrice Nakibuuka
In hospitals, homes and even on busy streets, there are moments when a person suddenly stops breathing or their heart stops beating. In such emergencies, health workers and trained bystanders may rush to perform a life-saving procedure known as resuscitation.
For many people, resuscitation is something they have only seen in movies where doctors shout instructions and press on a patient’s chest while machines beep loudly. In real life, however, the process is more structured, guided by medical protocols and often determines whether someone lives or dies.
Understanding what resuscitation is, when it is used and its limits can help communities appreciate its importance and why learning basic life-saving skills matters.
What is resuscitation?
Resuscitation is a medical procedure used to restore breathing or blood circulation when a person’s heart or lungs stop working properly.
In simple terms, it is an attempt to bring someone back from a life-threatening state such as cardiac arrest, severe breathing failure or unconsciousness.
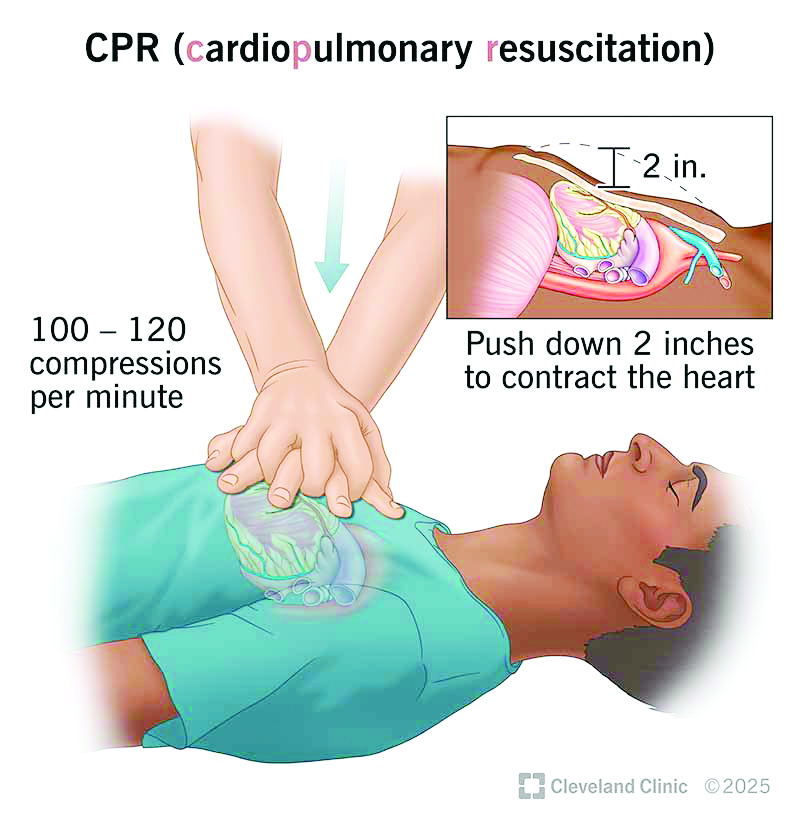
One of the most widely known forms of resuscitation is cardiopulmonary resuscitation (CPR). This technique involves pressing firmly on the chest and sometimes giving rescue breaths to keep blood and oxygen moving through the body until the heart can start beating again.
Doctors say the goal of resuscitation is to keep oxygen flowing to the brain and other vital organs. Without oxygen, brain cells can begin to die within four to six minutes.
“Resuscitation is about buying time for the body. By keeping blood circulating, we increase the chances that the patient can recover while we address the underlying cause of the emergency,” explains Dr Doreen Alaleit, an emergency physician at Mulago National Referral Hospital.
Situations that require resuscitation
Resuscitation may be needed in several medical emergencies.
One common situation is cardiac arrest, where the heart suddenly stops beating. This may happen because of heart disease, electric shock, severe trauma or certain medical conditions.
Another situation is when someone stops breathing due to drowning, choking, severe asthma attacks or drug overdose.
Resuscitation may also be performed on newborn babies who fail to breathe immediately after birth. In maternity wards, trained midwives often act quickly to help such babies begin breathing.
In accident scenes, health workers may perform resuscitation on victims who are unconscious or severely injured.
The faster resuscitation begins, the better the chances of survival. This is why health experts encourage members of the public to learn basic CPR skills.
How resuscitation is done
The exact method used during resuscitation depends on the patient’s condition and the setting.
In most cases involving cardiac arrest, the first step is CPR. The rescuer places the heel of their hand on the centre of the patient’s chest and presses down repeatedly. These chest compressions help pump blood through the body when the heart is not beating effectively.
Rescue breaths may also be given by blowing air into the patient’s mouth to provide oxygen.
In health facilities, medical teams may use additional equipment to support resuscitation. These may include oxygen masks, breathing tubes, suction machines and medications that stimulate the heart.
Another important tool is the defibrillator. This device delivers a controlled electric shock to the heart in certain types of cardiac arrest. The shock can help restore a normal heart rhythm.
Emergency teams usually follow internationally recognised resuscitation protocols that guide them step by step during such situations.
“The process may look chaotic to an observer, but every member of the team has a specific role,” Dr Alaleit says, adding: “Someone performs chest compressions, another manages the airway, another monitors the patient and administers drugs,”
Resuscitation in newborn babies
Resuscitation is not only performed on adults. In delivery rooms, it can be a critical intervention for newborns who do not begin breathing immediately after birth.
Midwives and doctors are trained in neonatal resuscitation techniques. These may include clearing the baby’s airway, gently stimulating breathing or providing oxygen support. Most babies respond quickly to these interventions.
“In many cases, a baby simply needs stimulation and assistance with breathing,” explains a midwife at a maternity clinic in central Uganda. “But if help is delayed, the baby can suffer brain damage due to lack of oxygen.”
Training birth attendants in neonatal resuscitation has significantly improved survival rates for newborns in many countries.
When resuscitation may not work
Despite medical advances, resuscitation is not always successful.
Several factors influence whether it works, including the cause of the cardiac arrest, the patient’s overall health and how quickly the intervention begins.
If the brain has been without oxygen for too long, the chances of survival decrease dramatically. Even if the heart starts beating again, the patient may suffer severe brain injury.
Certain conditions also reduce the chances of successful resuscitation. These include advanced cancer, severe infections, major organ failure or extensive trauma.
In some cases, the heart cannot respond to treatment despite repeated attempts by the medical team.
“It can be very difficult for families when resuscitation fails. But sometimes the body has simply reached a point where recovery is no longer possible,” Dr Alaleit says.
When resuscitation may not be attempted
There are also situations where doctors may decide not to attempt resuscitation.
For example, if a patient has a terminal illness and resuscitation would not improve their quality of life, medical teams may follow a “do not resuscitate” order.
A do-not-resuscitate instruction is usually discussed between doctors, patients and their families in advance. It means that if the patient’s heart stops, the medical team will focus on comfort care rather than aggressive resuscitation.
Such decisions can be emotionally difficult but are often guided by ethical considerations about dignity and suffering.
Doctors also consider whether resuscitation would cause more harm than benefit. For frail elderly patients with multiple illnesses, aggressive resuscitation may result in painful injuries such as broken ribs without significantly improving survival chances.
Ethical considerations in resuscitation
Resuscitation raises important ethical questions in medicine.
One key issue is patient autonomy, the right of individuals to decide what kind of medical care they want.
Some patients choose not to undergo resuscitation if their condition is severe and recovery is unlikely. Others request that every possible effort be made to save their lives.
Doctors must respect these wishes while also considering what is medically appropriate.
Another ethical concern involves the allocation of medical resources. In overwhelmed health systems, doctors sometimes face difficult decisions about which patients are most likely to benefit from intensive care.
Clear communication between doctors, patients and families is essential in making these decisions.
Effectiveness of resuscitation
Although resuscitation does not always succeed, it has saved many lives.
Studies from emergency medicine show that immediate CPR can double or even triple the chances of survival in certain cardiac arrest cases.
However, survival rates vary widely depending on the circumstances.
Cardiac arrests that occur in hospitals often have better outcomes because medical equipment and trained personnel are readily available.
In community settings, survival depends heavily on whether bystanders recognise the emergency and start CPR before professional help arrives.
Public training programmes in CPR have therefore become an important part of improving survival rates.
Importance of public awareness
Health experts emphasise that ordinary people can play a crucial role in saving lives through basic resuscitation skills.
Learning how to recognise cardiac arrest, call for help and CPR can make a significant difference during emergencies.
In many countries, CPR training is included in school programmes and community health initiatives.
“In emergencies, the first few minutes are critical. If someone nearby knows how to start chest compressions while waiting for an ambulance, it can save a life,” says Dr Aleleit.
Increasing awareness about resuscitation can also help communities understand its limitations and reduce unrealistic expectations.
A race against time
Resuscitation represents one of the most dramatic and urgent moments in medicine. It is a race against time, where doctors, nurses and sometimes ordinary bystanders work together to restore life.
While it does not guarantee survival, it remains a vital medical intervention that has saved countless lives.
Understanding what resuscitation involves and recognising both its power and its limits helps communities appreciate the complexity of emergency medicine.
Ultimately, the goal is simple: to give patients the best possible chance to live when every second counts.